The Science behind our Asthma Therapy
Our technology is based on years of research into the lung structure and function. Below we will outline a few key aspects of the lung structure in asthma that our drug aims to target.
Why Lung Structure Matters in Asthma
Lung Structure
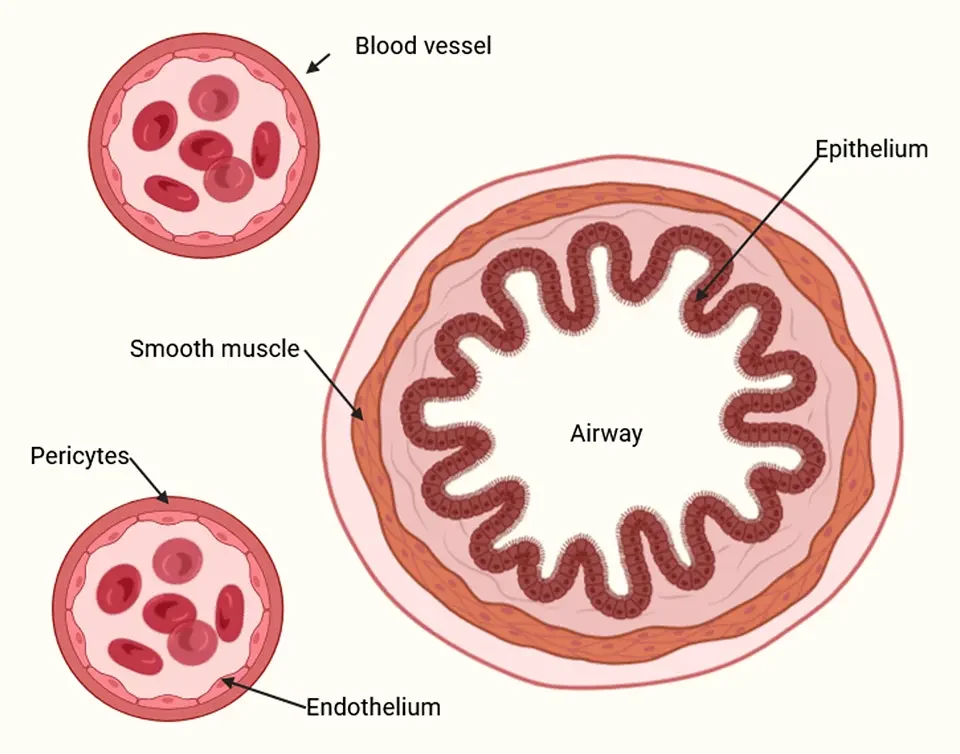
Asthma is a disease of the large and small airways. Airways consist of a layer of epithelial cells, which act as a barrier to airborne particles, and a layer of smooth muscle, which constricts and relaxes, allowing us to breathe in and out.
Blood vessels are often found near airways and are comprised of a layer of endothelial cells, which form the barrier of the blood vessel and pericytes, which regulate the vessels and provide structural support.
Cellular Disruption in the Asthmatic Lung
In Asthma
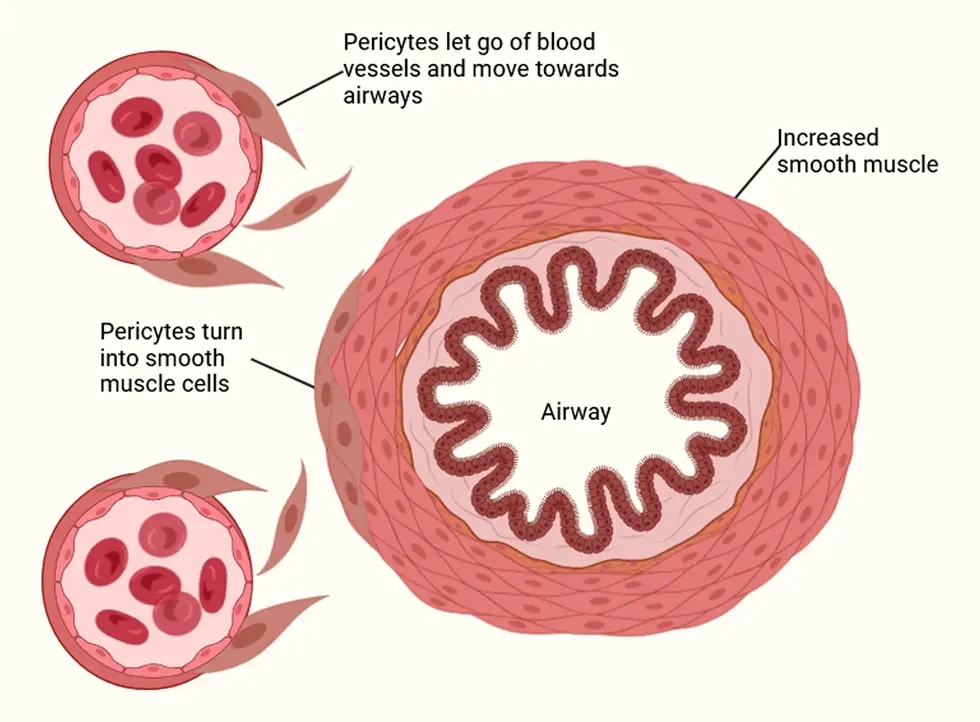
In an asthmatic lung, normal cellular processes are disrupted. Pericytes become detached from the blood vessels and migrate towards the airway. This results in a leakier blood vessel, allowing more immune cells to enter from the bloodstream.
At the airway, pericytes differentiate into a cell called a myofibroblast, which creates a thicker smooth muscle layer, causing shortness of breath and wheezing.
In addition, these myofibroblasts also release proteins which clog up the airway, making it even stiffer.
Chemotaxis and Asthma Progression
Chemotaxis
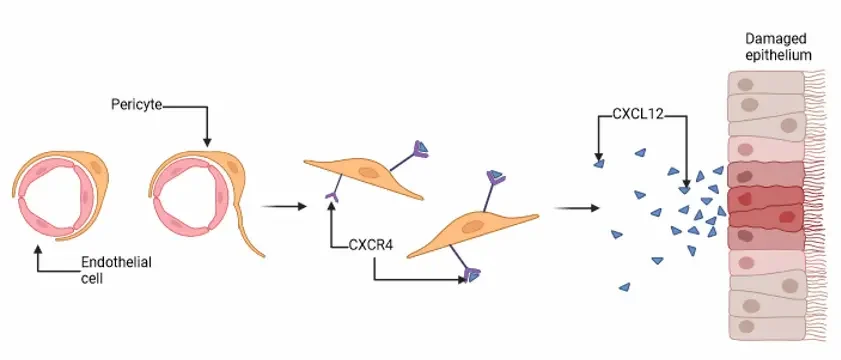
Chemotaxis is the movement of a cell in response to a chemical stimulus. In this case, it is the movement of pericytes towards a high concentration of a molecule called CXCL12.
We know that there is a high concentration of CXCL12 molecules near damaged airways and a low concentration of CXCL12 near blood vessels. Therefore, pericytes follow this trail of breadcrumbs towards the airway.
This phenomenon is likely to be a dysregulated wound healing response, as pericytes often migrate towards wounds, differentiate into myofibroblasts, and release the proteins that cause scar tissue.